Reintegration of Burn Patients into Society and Home
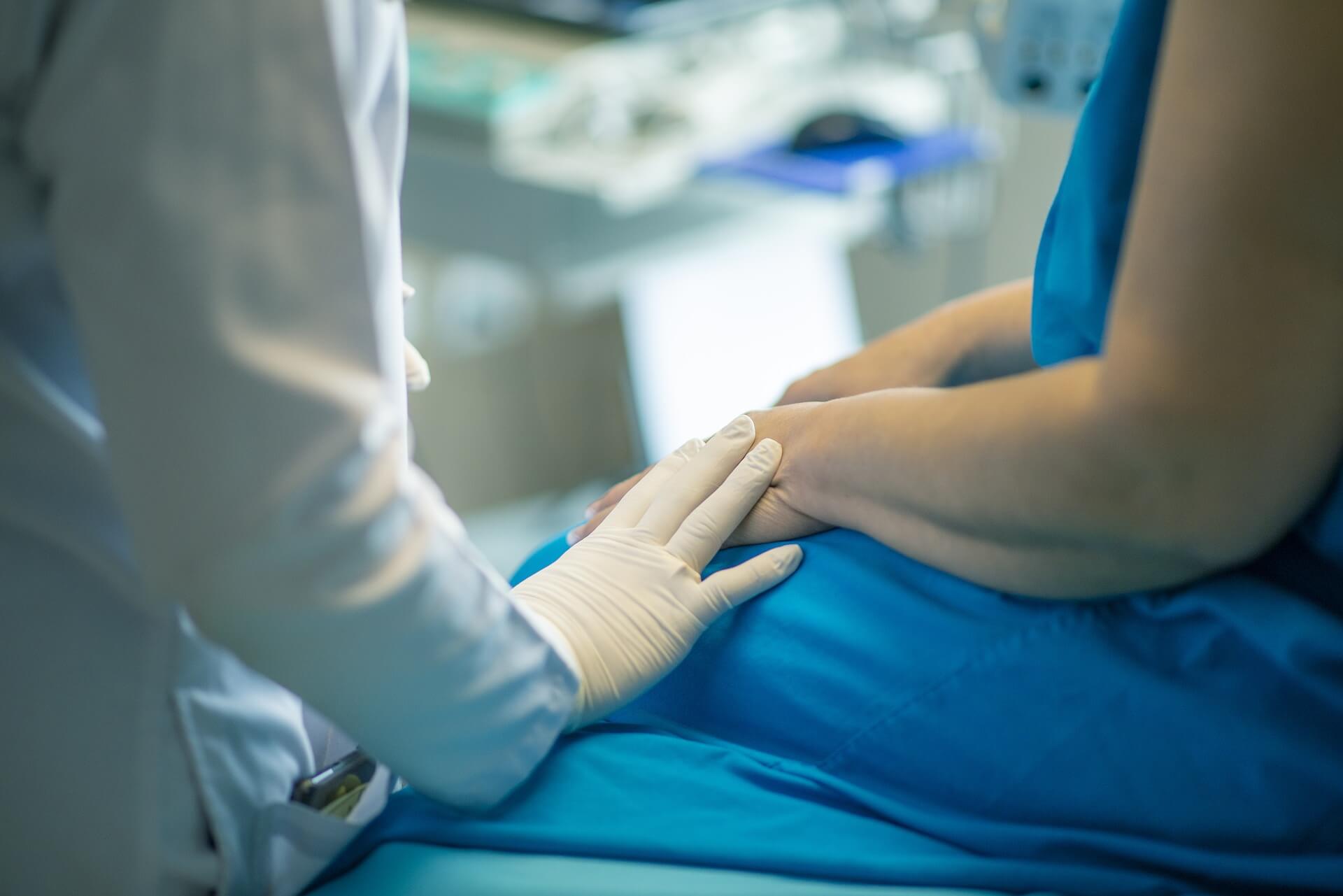
People with severe burns undergo major psychological and physical trauma that impacts the ability of the person to bounce back as a functional member of society. These are patients who suffer from body image problems, depression, post-traumatic stress, grief, chronic itching, and chronic pain, all of which interfere with the patient's overall functioning. Work and family responsibilities can suffer greatly. On the good side, many burn patients are resilient and suffer few long-term consequences of their burn injury.
In the beginning, patients with burns often suffer from prolonged grieving. They grieve the loss of function and the change in their physical appearance. They are uncertain how long the hospitalization will be and are often separated from their social support group while in the hospital. Mental health professionals are necessary parts of the burn team so they can assist in helping the patient overcome their grief and face their new life after sustaining the burn.
Patients suffering from traumatic grief often have PTSD and anxiety along with it. They may also face the loss of loved ones, including beloved pets, who perished in the same fire or accident as the burned patient. It is up to mental health professionals to know when the right time is to reveal the news about these kinds of losses so the patient can properly process the grief.
Different cultures handle burn injuries differently. Even people who live and work in the same vicinity of the hospital must be able to handle the culture shock of having a patient (or being a patient) in a hospital, often for long periods. Becoming cultured in the hospital environment is trickier in patients who live far from the burn unit or have had to be treated in a different country than their country of origin. Dealing with being in a different culture with possible language barriers and other social barriers can contribute to poor recovery. It is up to the staff to try and bridge the gap between the hospital environment and the culture the patient and their family comes from.
Shortly after being hospitalized, a mental health worker needs to determine the patient's pre-injury state. This can be done by interviewing the patient and/or family members. There may be risk factors associated with pre-existing family problems that complicate long-term recovery. The family system will be the one the patient is healing in after being discharged from the hospital.
Critical Care PhaseInitially, there is often what is known as an admission crisis. It involves the patient and family struggling with terror, shock, disbelief, pain, anxiety, and confusion. The family may believe that the patient is near death. This is the time to establish a therapeutic rapport with the patient and their family so that communication can go back and forth between patients, families, and staff more efficiently.
The first two jobs are to get the patient-oriented to the new environment and recognize what has happened to them. The patient and family must quickly believe that they are in good therapeutic hands to maximize their cooperation with the staff. Repeated statements of reassurance may be necessary to calm all of those involved. It is essential to recognize that both the patient and their family suffer from an acute traumatic response. Both must be handled carefully and with full attention to their psychological needs.
In the critical care stage, both the patient and family will need lots of reassurance and knowledge about what is happening. This is the stage when many procedures are being done to repair the burn, which can overwhelm the individuals involved. Communication about what is going on is crucial. Anxiety and pain must be handled most effectively until the patient is past the critical phase of care. Some hospitals use music therapy, meditation, visualization, and other alternative techniques to distract the patient during procedures. Even having a close family member on hand for practice can reduce the anxiety and pain the patient is likely to feel. Both children and adults can benefit from these types of alternative therapies.
Rehabilitative Phase of HealingAs the patient begins to heal, more education will be necessary, and time must be given for the patient and family to adjust to new roles. Alternative therapies like meditation and progressive relaxation will continue to be required, and adequate pharmacological control over the individual's pain and anxiety. Many patients regress during this phase, and this is particularly true in children. Children can develop unhealthy behaviors, and the parents will need to know that this is a part of the normal recovery process from a severe burn.
Many patients and family members struggle with what will happen in the future as the patient recovers. This provides an opportunity for staff and mental health workers to educate the patient on the mental, emotional, and physical issues that can be dealt with over time.
Reintegration into the Patient's Normal LifeThe patient and family must cope with potentially permanent changes in their lives and can be helped through this with psychotherapy. The family needs to be educated on what can happen as the patient is reintegrated into their everyday life. Social skills programs can be offered to help the patient handle different social situations that occur during the patient's reintegration.
Individuals who return to work tend to recover faster and have greater coping strategies. Research has shown that about 65 percent of burn patients with severe burns eventually return to work within two years. These people need confidence and social support around returning to work.
The patient is still susceptible to delayed grief reactions, anxiety states, and post-traumatic stress disorder after leaving the protective environment of the hospital. Most will need ongoing psychotherapy to get through the initial months and years after sustaining a severe burn. Body image difficulties and social stigmatization can make the reintegration phase much worse.
Evidence suggests that most burn patients adjust to their new lives post-burn after about two years. During this time, psychotherapy and medical management of their psychological condition can stabilize the patient so that their quality of life can be as good as possible. The trick is to find appropriate mental health professionals who have knowledge about treating burn victims and their emotional problems. Mental health treatment is. However, expensive and too many burn victims do not have insurance to cover this kind of mental help.
Sacramento Burn Injury LawyerIf you have sustained devastating burn injuries, call our experienced Burn Injury Attorneys in Sacramento today for free and friendly case advice at (916) 921-6400 or (800) 404-5400.
See our history of settlements and verdicts.
We are a member of the Million Dollar Advocates and the Top One Percent
Editor's Note: This page has been updated for accuracy and relevancy. [cha 5.27.22]
Image from Pixabay by fernando zhiminaicela [cs 1137]