Sacramento Thoracic Disc Injury Lawyer
Your Thoracic Disc Injury Attorney in Sacramento
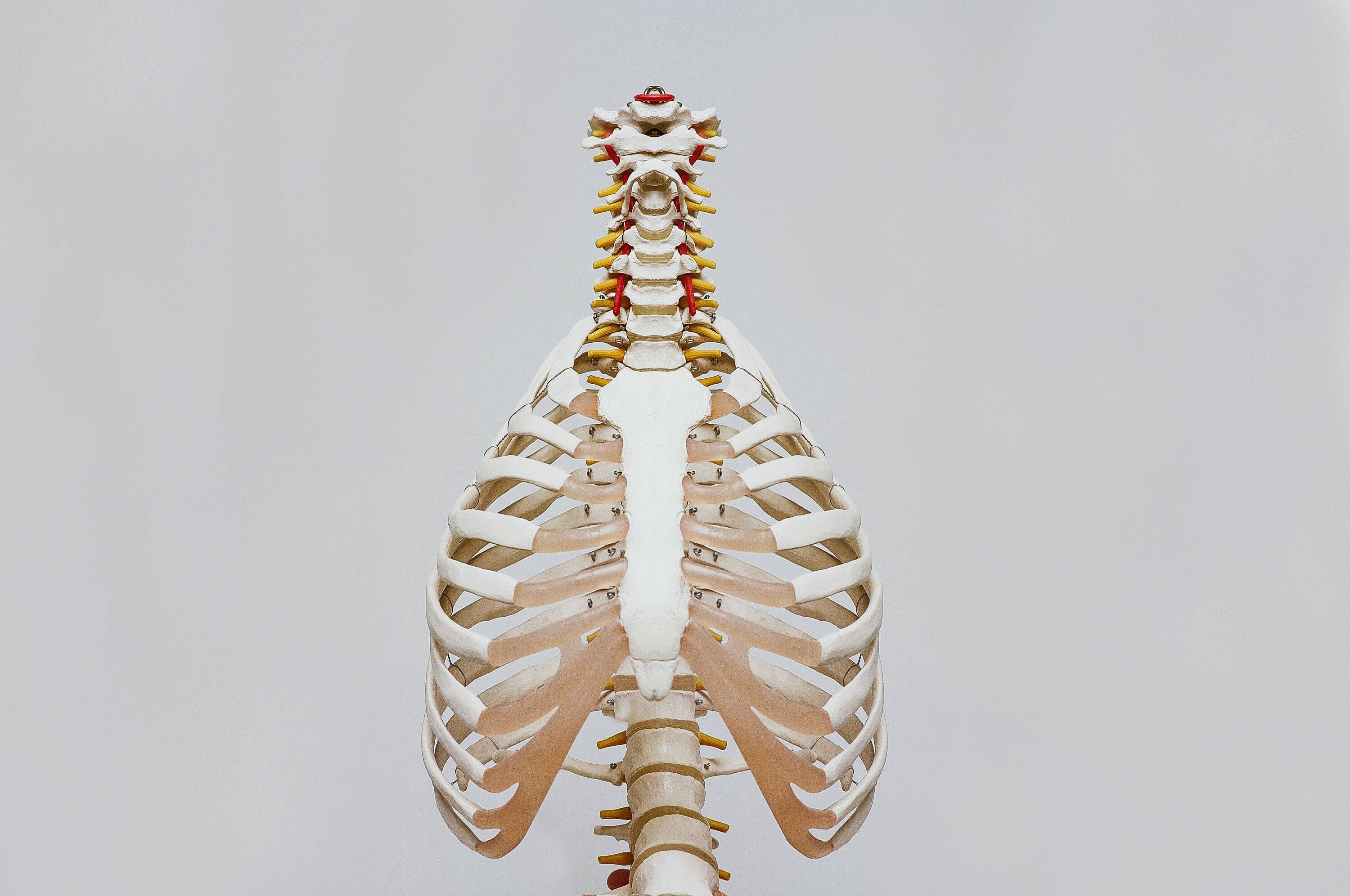
Intervertebral (IV) discs allow for the articulation of the superior surface of the inferior vertebral body with the inferior surface of the superior vertebral body. There are twenty-five in total, with one in the sacral region, five in the lumbar region, seven in the cervical region, and twelve in the thoracic region. These comprise approximately one-quarter to one-third of the length of the spine. IV discs allow for the flexibility of the spine without a compromise of strength in addition to providing a shock-absorbing effect from the prevention of the vertebrae from grinding with one another. The structure of the IV discs is composed of three major components that include the cartilaginous endplates, the annulus fibrosus (AF), and the nucleus pulposus (NP). An injury to the thoracic region may result in a herniated disc from damage to the annulus fibrosus and rupturing of the nucleus pulposus.
If an accident left you with a herniated thoracic disc, call us today at (916) 921-6400 or (800) 404-5400 to speak with one of our personal injury lawyers in Sacramento. We have handled cases like yours since 1982 and would like to put our experience, skills, and resources to work for you.
A serious accident may change your life forever. At AutoAccident.com, we are here to help you obtain the justice and fair compensation you need and deserve after being injured in a crash caused by another party or entity’s negligence. Our law firm has fought to protect the rights and interests of our clients for over three decades. You can depend on us to put our knowledge and expertise to work for your thoracic disc herniation case. We understand the emotional, financial, and physical devastation that may accompany a collision and the challenging battle that may arise when dealing with difficult insurance companies and defense counsel. Fortunately, you do not have to go through it alone. Give us a call today to schedule a free consultation with one of our accident attorneys to go over the details of your personal injury case and learn how we can help you and your family.
What is a Herniated Disc and How Does it Happen?A herniated disc refers to a condition that occurs because of a displacement of the nucleus pulposus from the intervertebral space. It is often referred to as a bulging, ruptured, or slipped disc. While rare, it mainly occurs between L1 and T8. In some cases, disc herniation in the thoracic region may result in the compression of the spinal cord or nerve that leads to pain that is consistent with spinal cord dysfunction or nerve compression. Such conditions are also known as myelopathy.
Herniated discs generally occur from wear and tear from the loss of elasticity within the spinal discs. This may cause the fluid to leak out of the spinal discs and result in brittleness or cracking. While such changes are considered normal in the aging process, they may vary in extent from patient to patient. In some extreme cases, a serious injury or an accident may cause trauma to the spinal disc and result in herniation.
How Do You Know if You Have a Herniated Thoracic Disc?The signs and symptoms of disc herniation within the thoracic region may include:
- Certain muscles of one or both legs may experience weakness
- Pain is often described as stinging or burning that may radiate into the lower extremities
- Spasticity in one or both legs from increased reflexes
- Tingling or numbness in one or both legs
It is not uncommon for a patient presenting with a herniated disc to not experience any symptoms. For asymptomatic patients, diagnostic imaging may be necessary to show the exact location of the herniation and its severity.
How is a Thoracic Disc Injury Diagnosed?Diagnosis of a herniated disc in the thoracic spine generally includes an evaluation of patient history and a physical exam. It may also be supplemented by diagnostic imaging to assess nerve root compression because of disc herniation in patients presenting with leg pain or back pain. Diagnostic tests may also be utilized in the identification of the affected disc and its severity before surgical intervention. These may include:
- Magnetic Resonance Imaging (MRI): The imaging modality of choice for thoracic disc herniation cases is MRI. It is considered the most useful imaging tool in the identification of disc pathology as it is the most accurate and painless test.
- X-Ray: A plain X-ray may not show disc herniation in the thoracic region of the spine. However, this diagnostic test may be utilized in the identification of spinal instability and localization of injuries in trauma cases.
An MRI and X-ray may not tell the whole story of the traumatic injury. Other diagnostic tests such as a CT scan or myelogram may be necessary as some disc herniation cases require surgical management. That is why it is essential for prompt diagnosis through medical imaging.
How is Thoracic Disc Herniation Treated?Non-surgical treatment of a disc herniation in the thoracic spine may include activity modification, a short period of rest, and the application of ice packs to the affected area as often as needed. To treat the symptoms, a physician may recommend analgesics for pain management. Rehabilitation such as chiropractic treatment may also be useful for manual manipulation of the injured area. A patient may also seek temporary relief for pain through a thoracic epidural injection.
Is Surgery Necessary for a Herniated Disc in the Thoracic Spine?A physician may recommend surgical intervention in cases where a patient has neurological deficits, intercostal neuralgia, or severe back pain. A laminotomy and discectomy are most often recommended in thoracic disc herniation cases requiring surgical management. It involves making an opening in the lamina and removing the herniated disc. The incision is generally made down the center of the back over the affected area, the muscles are moved to the side for the surgeon to have better viewing of the rear of the vertebrae, and a small opening is made between the two vertebrae surrounding the disc herniation. The removal of the disc may relieve any irritation or pressure on the spinal nerves.
What are the Possible Complications of Thoracic Disc Herniation?The risk of complications is often reduced by thorough pre-operative planning. Conversely, some of the possible complications from a herniated thoracic disc may include:
- A disc herniation may result in degenerative disc disease that may take several years for the condition to develop
- Chronic pain from the incomplete recovery of the nerves damaged by the pressure that is placed on them from disc herniation
- Complete paralysis below the waist from a rupture within the spinal canal because of a fragment of disc material
- Infection may occur within the disc area, spinal canal surrounding the nerves, and the skin incision
- Nerve injury from the removal of a herniated disc while a surgeon is operating near the nerves of the spine and thus, resulting in numbness, pain, or weakness in the affected area
- Permanent nerve damage within the lower body and extremities from spinal cord pressure resulting in bladder and bowel dysfunction
Only a physician may evaluate a patient’s condition and inform them of the risks that may accompany any conservative treatment or surgery they may recommend.
Can You Seek Compensation for Injuries from an Accident?A party involved in an accident may be entitled to compensatory damages for any injuries that were the direct result of the incident through a bodily injury claim. This may include financial and intangible losses such as medical bills, lost earnings, loss of consortium, pain and suffering, and more. In the case of thoracic disc herniation, out-of-pocket expenses such as modifications to the home to accommodate a permanent injury or disability, costs of future medical treatment, and loss of future earning potential should all be considered.
The recovery process usually involves bringing a claim with the insurance company representing the at-fault party. However, it is not always straightforward as there may be disputes regarding fault and the extent of damages. The insurer should not have the final say in how much a personal injury claim is worth. Therefore, it is essential to work with an injury lawyer with years of experience handling thoracic disc herniation cases to ensure that you are fairly compensated for your losses.
What Effects Does a Pre-Existing Injury Have on an Accident Case?A pre-existing condition is a health issue or injury that affected a party before they were hurt in an accident. If a pre-existing condition was aggravated or worsened because of an accident, a claimant may seek compensatory damages for the impact the incident has had on their life. In other words, if an injured party without degenerative disc disease suffered a thoracic disc herniation in a crash, they may be able to seek compensation for economic and non-economic damages without the consideration of a pre-existing condition.
Keep in mind that it is not uncommon for the insurance company to make a lowball settlement offer or outright deny a bodily injury claim. That is because they will do anything in their power to limit their financial liability in a crash caused by their insured. The same may be said in first-party claims brought through an injured party’s uninsured and underinsured motorist (UM and UIM) coverage. While we would all expect the insurance carrier to make things right and fairly compensate a party injured in a collision for the undue harm they have endured, that does not always happen in all cases.
It is essential to retain legal counsel after suffering a thoracic disc herniation in an accident to ensure that the insurer will not take advantage of you and your situation. Such cases may be challenging to present to a jury, and without an experienced thoracic disc injury lawyer, you may be making a costly mistake. Finding the best accident attorney to represent you may be tough, particularly if you are unsure of what to look for in a lawyer. For information on how to select the right attorney to handle your personal injury case, watch this video.
Contact a Thoracic Disc Injury Attorney TodaySeeking financial compensation after an accident may be challenging, particularly when injuries such as thoracic disc herniation are involved. The time after the incident may often result in mounting medical expenses, wage loss, and other losses. Thankfully, California understands the emotional, physical, and financial hardship that may result from a crash and provides injured parties a way of seeking relief through an injury case. Before determining your next steps, you should discuss your case with an experienced accident attorney for help understanding your rights as a claimant.
Over the years, our law firm has handled many injury cases arising from all types of accidents. If you have suffered thoracic disc herniation because of a crash caused by another party or entity’s negligence, please call us today to discuss your case at (916) 921-6400 or (800) 404-5400. We are available anytime to provide free, friendly advice on some of the options that may be available to you in your situation.
Photo Source: By “Nino-Liverani” via Unsplash
:ds [cs 1879] bw