Orbital Fracture Lawyer
Orbital Fracture Lawyer
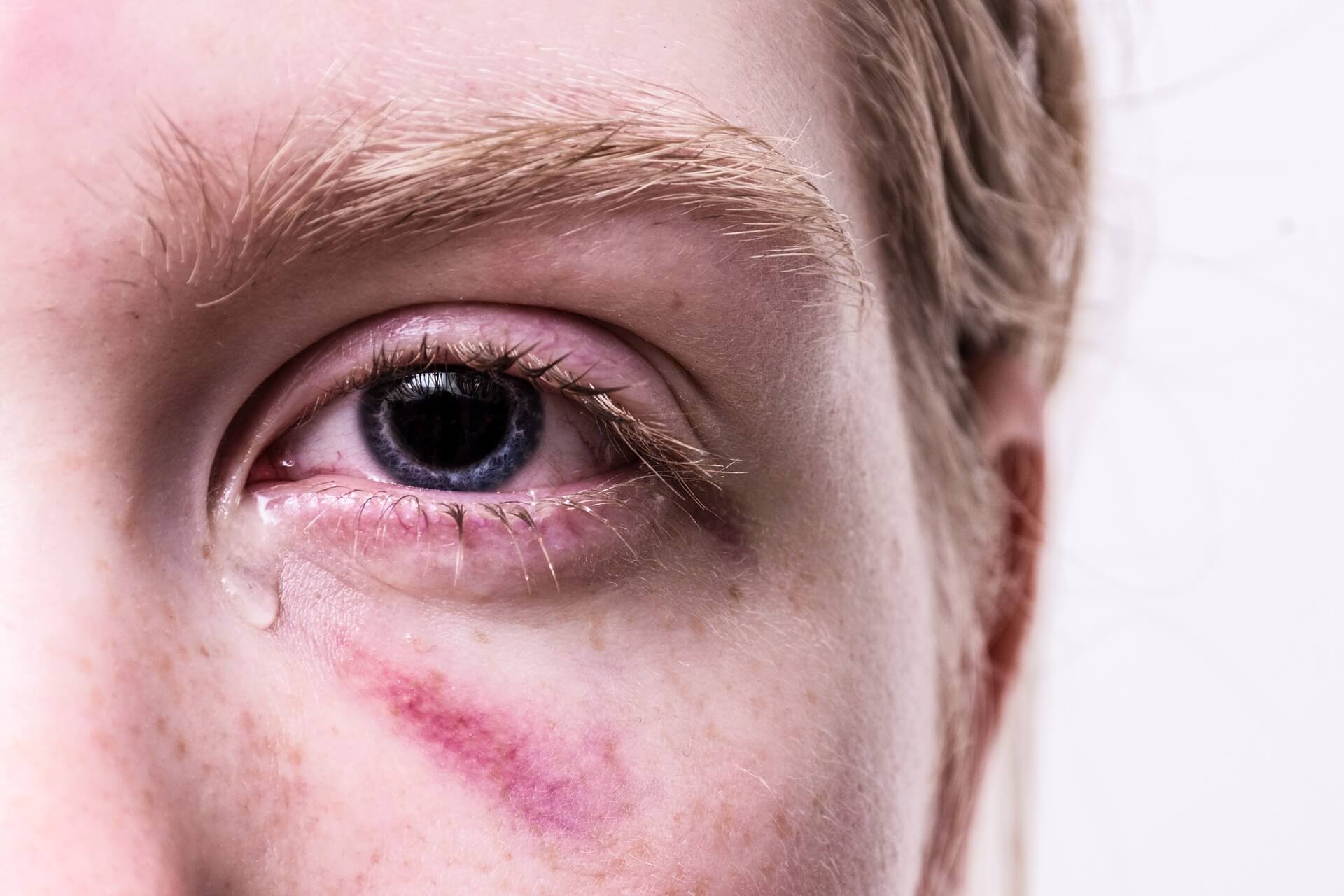
An orbital fracture results from a break in one of the bones around the eyeball (eye socket or orbit). This type of bone fracture is caused by an object striking the eye with substantial force. Such injuries are considered some of the more challenging for plastic surgeons. As a prominent feature of the face, the most minor asymmetries may be devastating to the affected patient. In treatment, physicians must consider specific aspects of both diagnostic procedures and management in obtaining optimal results.
If you or a member of your family has suffered a serious injury in an accident, such as an orbital fracture, contact our personal injury attorneys in Sacramento today at (916) 921-6400 or (800) 404-5400. We are available anytime to review the details of your case and provide free, friendly advice.
Our law firm has been helping California families affected by catastrophic accidents since 1982. Unlike the insurance company representing the at-fault party, we will have your best interests at heart. We are dedicated to obtaining the justice, and fair compensation injured parties deserve. Contact our personal injury lawyers today to learn more about how we can help you and your family.
What are the Types of Orbital Fractures?The bones around the eye may fracture or break in the event of an accident. The types of eye socket fractures are as follows:
- Blowout: A blowout fracture involves a break in the inner wall or floor of the eye socket or orbit. These walls comprise fragile bone, and any crack may cause pinching on muscles and other structures surrounding the eye. This may lead to the inability to move the eye normally. Being struck with a fist or a baseball is often the cause of a blowout fracture. Another mechanism of injury may be an auto accident.
- Orbital Floor: This type of injury occurs when trauma or a blow has pushed the bones of the orbital rim backward. This may cause the bones of the eye socket floor to buckle downward. It may also involve the medial wall. Such fractures may also impact the nerves and muscles around the eye, preventing it from feeling normal and moving properly. In the elderly, such fractures may occur when a fall causes the cheek to strike a hard surface object.
- Orbital Rim: This type of fracture affects the eye socket and its bony outer edge. Since the orbital rim comprises thick bone, trauma to this area must have substantial force for a break to happen. Traffic collisions are some of the most common causes of orbital rim fractures. If a patient has sustained a break in the orbital rim, there is a possibility of other injuries optic nerve and the face.
The symptoms of an eye socket fracture will vary on the type of break and the severity of the eye injury. Symptoms may include the following:
- Blood in the white area (sclera) of the eye
- Bruising around the eyes that is blue or black in color
- Bulging or sinking of the eyeballs
- Decreased, blurry, or double vision
- Experience of intense pain in the cheek when opening the mouth
- Issues with moving the eye to look up, down, left, or right
- Numbness in the injured area of the face
- Swelling in the cheek, forehead, or skin under the eyes
A profound understanding of the pathophysiology and anatomy of an eye socket fracture is essential to successful management and restoration of the preoperative state for the patient. An ophthalmologist will check for an orbital fracture by examining the eye and the areas surrounding it. Images will be taken of the eye and the eye socket, including CT scans and X-rays.
The treating physician will also inspect the eye and determine whether it is moving normally and any vision issues. Measurements of the eye may also be taken to evaluate whether it is in the proper position in the eye socket.
Types of Treatment for Orbital FracturesAccording to the American Academy of Ophthalmology (AAO), surgical intervention is not always necessary in most eye socket fractures. An ophthalmologist treating a small orbital fracture may recommend ice packs placed over the injured area to allow the eye to heal on its own and reduce swelling. The treating physician may also prescribe decongestants and antibiotics. During the recovery process, patients are advised to avoid blowing their noses.
A severe case of an orbital fracture is when it repositioned the eyeball in the eye socket, causes double vision, or prevents the eye from moving as it should. In such situations, the patient may receive a referral from their ophthalmologist to an oculoplastic surgeon, an ophthalmologist specializing in surgery.
In most cases, oculoplastic surgeons will wait for the healing process for a brief period before performing surgery. Better outcomes often result from waiting for swelling to go down before surgical intervention. If symptoms of the eye socket fracture go away, it may be possible there may not be any related complications and the need for surgery.
Types of Personal Injury Compensation for an Eye Socket FractureSeeking full and fair compensation for losses resulting from a motor vehicle crash or another type of accident may be a challenging process. The purpose of damages in a personal injury claim is to make an injured person whole again. Depending on the circumstances and facts in the case, the claimant may seek recovery of economic and non-economic damages.
Economic damages consider monetary losses stemming from accident-related injuries and are calculated based on receipts and other records. Conversely, non-economic damages are challenging to place a value on as they are subjective in nature. Following are the types of economic and non-economic damages recoverable in bone fracture cases:
- Medical expenses
- Lost wages
- Loss of future earning capacity
- Disfigurement and scarring
- Emotional distress
- Pain and suffering
- Loss of consortium
- Out of pocket expenses for accident-related injuries
Keeping a record of all expenses and losses associated with the accident is essential for a successful claim. Conversely, various factors may impact the value of the case. To learn what these are, watch the video below.
What is the Statute of Limitations to Bring a Personal Injury Lawsuit in California?In California, there is a statute of limitations that applies to personal injury cases. This sets the period when a claimant may file a lawsuit in civil court against all at-fault parties. Under California Code of Civil Procedure Section 335.1, a lawsuit must be filed within two years of the accident date. Different time limits apply to other cases, such as medical malpractice and claims against government entities. Not meeting the deadline may result in case dismissal by the court.
Can a Preexisting Condition Affect a Personal Injury Claim?The existence of a preexisting condition may have a considerable impact on the value of a personal injury claim for an eye socket fracture. As the name suggests, a preexisting condition the patient suffered from before the injury or catastrophic accident in question.
When it is discovered that a patient’s condition has worsened because of a crash, the at-fault party may only be held liable for the worsening of the preexisting condition, not the underlying one that existed before the incident. The issue in such cases is that it may be challenging what problems and limitations are related to the preexisting condition and which ones have resulted from the collision.
Since the negligent party may only be held financially accountable for the injuries and damages they have caused, an individual presenting with a preexisting condition needs to compile evidence. This must establish that the subsequent accident has caused worsening of the preexisting condition. Medical records are one form of evidence that may be used to prove that.
Importance of Working with a Personal Injury AttorneyAn attorney who is experienced in handling personal injury matters will know the best way to identify and obtain medical records and other evidence necessary to prove accident-related injuries and damages incurred. A skilled injury lawyer will also advise the injured party of the potential challenges that may present in their case against difficult insurance companies, such as the defense tactics insurers use to dispute the value and validity of claims. An attorney will also work to ensure all filing criteria and deadlines applicable to the case are met.
One of the best steps to ensure you receive fair compensation is to hire an attorney as soon as possible. Any delay in retaining an attorney may limit their ability to conduct an independent investigation of the accident to determine fault and resulting damages. A lawyer can handle all aspects of the case to ensure that no mistakes are made, such as signing any documents or agreeing to any recorded statements with the insurer, which may impact the case.
Contact an Orbital Fracture Attorney TodayA catastrophic accident may be life-changing for the injured party and their family. In addition to property damage, injured parties may be dealing with serious injuries, such as eye socket fractures. The physical pain and emotional trauma may also cause immense stress for the affected person. The last thing anyone would want to worry about is dealing with difficult insurance companies, including your own, on personal injury claims. Our orbital fracture lawyers are here to help.
At our law firm, we have a history of obtaining successful results for families across California. When you hire us after an accident, we will handle all aspects of your case, so your focus will be on only taking care of yourself and your loved ones. Our legal team is available anytime to speak with you, explain what we can do for you, and provide free, friendly case advice. Contact us today to learn more at (916) 921-6400 or (800) 404-5400.
Photo Source: By “Anemone123” via Pixabay
:ds [cs 1661] cha